If you have diabetes, either Type 1 (insulin dependant) or Type 2 (diet or tablet controlled) you may have heard that it's not only your eyes that need special attention, but your feet too. In fact, it's really important to care for your feet at home on a daily basis, but also to visit a Podiatrist regularly too.
Diabetes is a condition that causes the body to not produce enough insulin. Insulin is a hormone produced in the pancreas which regulates the glucose (sugar) levels in the blood, stopping the level getting too high, or too low. If you have diabetes you will know that you have to try to maintain a steady blood sugar level, usually between 4-7 mmol/L, by controlling your sugar intake in food and drinks, taking regular exercise and taking your medication at the right times.
You know this already though, don't you?! That's why I've skimmed the surface here with the technical details of diabetes, Google has a wealth of information about it, but I want to talk about your feet, and how we can help you keep them in good health. You may have also been living with diabetes for a while and have been given all the advice you need from your GP, the practice nurse and the diabetic clinic.
I don't meet the NHS criteria for treatment, do I meet yours?
The problem is, the NHS is a changing service and many patients with diabetes are no longer being seen on a regular basis. This could be due to the increase in service users (patients) that the NHS has to see week in, week out. When a service reaches capacity, it either has to expand to keep up with demand, or it has to apply a new approach to see the patients who need to access the service because they have a higher need. We have had a recent influx of new patients to our practice who are experiencing problems with their feet, but do not qualify for NHS podiatry services as they do not meet the right criteria for treatment. We don't have any such criteria at Melton Podiatry Practice.
I don't need any more advice!
You really don't need any more advice, or leaflets, you've had enough of those already haven't you?! You're watching what you eat and checking your blood glucose levels, you're doing it all right, just like they told you to. But recently you've noticed you've got a strange sensation in one of your toes, it's not really a sensation, just a numbness with a bit of pins and needles. Or are you the chap who noticed that when you got into the bath last night you didn't know quite how hot the water was when you stepped in, until it reached your ankles and then you realised it was much too hot! Or are you the lady with diabetes who stepped on something sharp in the garden last week when we had that nice sunny weather and didn't realise you stepped on a thorn that's embedded in the sole of your foot now, unnoticed?
These are all common scenarios that us, podiatrists, hear about all the time. My personal favourite was the retired chap who came in the week after cutting his blackthorn hedge in his Wellington boots for his usual podiatry appointment to have his feet checked and nails maintained. He was quite suprised when I pointed out his big toe joint was very red and swollen; even more so when I removed a 5mm long blackthorn thorn and drained the wound. Antibiotics and several dressings later the wound healed, but he checked his feet for injuries and changes every day after that incident! Why had he not known the thorn was in his foot? His diabetes had caused neuropathy (loss of sensation) in his feet and he simply could not feel pain in certain area's anymore.
We don't need ALL the advice, we just need GOOD ADVICE! Great information, that we can digest and act on if we need to. A resource that we may not need right now, but one that we can call on when we do. We can give you that advice (and with a smile too!)
What do Podiatrists know about diabetes anyway?
I feel like I need to give you our C.V, as a profession, because lots of people don't really know what we do. Most people know us (Podiatrists) as Chiropodists, and with that title think we just cut toenails and remove corns. And you know what? That is part of what we do. I give those treatments on a daily basis to keep people comfy, but we do a LOT more. So here goes, let me tell you why we know about diabetes, and more so, about the diabetic FOOT!
If you see a bona fide Podiatrist, they will be degree trained (or previously hold the Diploma in Podiatric Medicine) and come with a Bachelor of Science Podiatry degree from one of the many schools of podiatry (universities) in the UK. We spend 3 years studying the foot and the lower limb. We learn about diabetes, it's impact on your body and importantly the problems it can cause in your feet and legs. We know how important prevention of the complications of diabetes in the foot are.
Each of our Podiatrists at Melton Podiatry Practice hold a BSc (Hons) Podiatry degree, have worked in the NHS and rotated through the Diabetic Foot Clinic at Ipswich Hospital gaining experience and knowledge in managing the diabetic foot and, finally, helping those with diabetes care for their feet. So we know quite a lot, it's all squirrelled away in our brains you see!
How do we detect problems in the diabetic foot?
Blood supply:
Good blood supply to the feet is carried by arteries from the heart and all the way down the leg and into the foot, right to the tip of your toes. Arteries should be elastic, capable of continuing the pumping of blood that the heart starts, all the way to the peripheries. The arterial blood is warm, full of oxygen and serves to nourish the tissues and skin. It also contains clever cells that fight infections from bacteria and germs, but also aids clotting when you cut yourself. It also nourishes hair and nail growth.
We have a clever little machine that lets us listen to the condition of the artery and the blood that is flowing through it. This machine is called a Doppler. It's hand held and the probe is laid onto the foot over the artery below the skin, allowing us to listen to the blood flow through that artery into your foot. There are two main arteries that we listen to; the dorsals pedis and the posterior tibial. We are also able to detect atrial fibrillation (AF) and peripheral arterial disease (PAD) during this test. If we find this we can liase with your GP for further investigation and treatment if necessary. It's not just the foot we are interested in you see, it's the whole of your body.
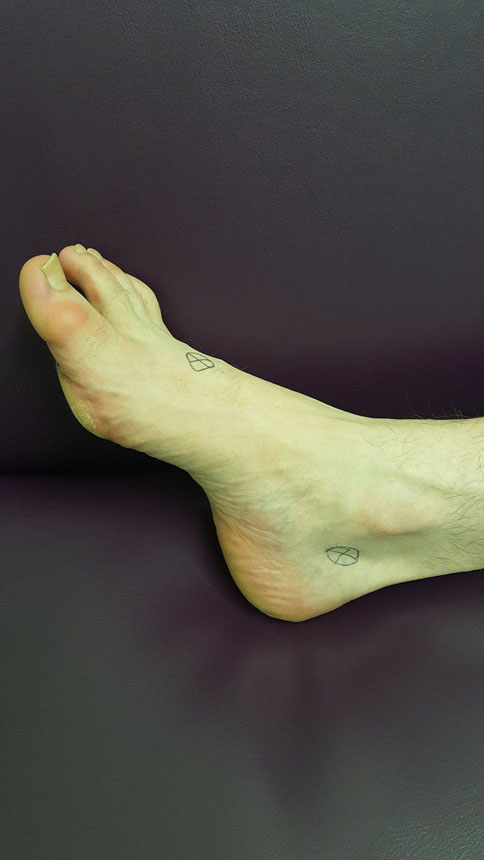
Sensation:
We have an array of tests to find out which types of nerves in your feet are functioning properly. We test the nerves that detect pain (which let you know you have trodden on something sharp or cut yourself), the ones that detect temperature (so you don't scald your foot when stepping into a bath before you have checked the temperature of the water for instance), the nerves that detect pressure (so if your new shoes rub your foot on the first wear, you definitely know about it) and the ones that detect vibration (giving feedback to your brain about where your foot is at any moment in time). I bet you didn't know you have so many nerves in your foot in the first place, let alone how they are responsible for protecting your foot from damage?!

- Low Risk: great circulation and no loss of sensation; you're less likely to injure your foot without knowing.
- Medium Risk: your circulation may not be as good as we would hope but you haven't lost any sensation in your feet; this may predispose you to slower wound healing if you injure your foot.
- High Risk: your circulation may be poor and you have also lost sensation in your feet too; this may mean that you are at higher risk of injuring your feet and once injured, the wound may heal very slowly or you may be at risk of ulceration, gangrene or amputation (the last two are quite dramatic outcomes, but they can and do happen).

